
Hayfever? 6 Steps to a Carefree Summer
Is this your field of dreams or source of sneezy nightmares? If you have hayfever you’ll certainly know which side of the fence you’re on. Now’s the time to make a change.
For the longest time I dreamed of not flinching or holding my breath when I walked past freshly cut grass. Of not wondering whether it was ‘safe’ to go outside. I got fed up watching people skippng through the park, tra-la-la-ing, without a hayfever-based care in the world. I even remember the time when I resorted to drinking hayfever eye drops, because I couldn’t take any more antihistamine that day and my throat JUST WOULD NOT STOP ITCHING.
That was when I thought… enough! Fed up with taking over-the-counter medications which just treated the symptoms I turned to a more natural arsenal. My goal was to not only target the effects of itch-inducing histamine, but also teach my immune system to be less hysterical and reactive at the first whiff of pollen.
Sometimes it gets to April and I think, “I must do something about my hayfever”. Then a week, or three, pass, suddenly it’s June, and BOOM – the sniffing, sneezing, itchy eyes and months of envy begin. And I start thinking of the many times I promised to do something about it.
But if June has come and I haven’t done any prep work then I really only have myself to blame. Why? Because I know that most of these natural remedies need a bit of time to take full effect.
That’s why April is such a key month, and the perfect time for this post. If you’re a hay fever sufferer like me, it gives you plenty of time to get ready. Get into the routine now, and you’ll be in a much better state when the pollen is swirling through the air, mid-June. Of course if your symptoms start earlier, say in May, then next year you’ll want to start prepping in March.
***
FIRST THINGS FIRST
Before we talk about these nutrients, I think it makes sense to quickly look into exactly what’s happening with hayfever. Know this, and you’ll be able to put together a core group of supplements which are broadly targeted and incredibly effective. We can also look at the supplements which are more suited for on-the-spot actions. In fact, I’ll cover this in a later post, so don’t forget to keep an eye out.
Hayfever Uncovered
Also known as allergic rhinitis, hayfever affects adults and children alike, between 10-30% of adults. The allergy season typically runs from Spring to early Autumn. Reacting to pollen from grass, trees and weeds, and even mould spores, sufferers commonly experience symptoms which include:
- Itchy eyes or throat
- Sneezing, blocked or runny nose
- Red or watering eyes
- Headache and blocked sinuses
- Shortness of breath
- Tiredness
What’s Going On In Hayfever
There are actually quite a few stages before you reach the tipping point, when the itching, sneezing and wheezing start.
- First pollen is released into the air, is breathed into the body, and gets misidentified as a ‘pathogen’. Very quickly, the body produces IgE antibodies, molecules which act as sentinels, looking out for future ‘attack’ from this harmless pollen.
- Next season, when the pollen is again released, it’s breathed in, and is deposited in connective tissue lining the air passages and gastrointestinal tract. This is where it encounters mast cells.
- Mast cells have an important role in the immune system – healing wounds and defending against pathogens. However, in hayfever sufferers they go slightly overboard. Primed and covered in IgE antibody, the mast cells sit and wait for an encounter with this ‘pathogenic’ pollen.
- As the days pass, more and more pollen is loaded on to the IgE antibodies covering the mast cell surface. Finally a tipping point is reached. The fully loaded antibodies cross-link, pulling apart the mast cell walls, releasing granules packed full of histamine and cytokines.
- Allergic symptoms only begin once these chemical mediators flood the environment. For instance, when histamine binds to receptors in the smooth muscle and the lining of blood vessels and airways, adding to the localised inflammatory response in these tissues.
Key Questions To Ask
Knowing this means we can start asking the right questions:
- Can the immune system be encouraged to respond appropriately to harmless pollen, and not misidentify it as a harmful pathogen?
- Can we slow down the rate at which pollen enters the system?
- Can we strengthen the walls of the mast cells, and delay the moment at which they split open?
- Can we dampen down the inflammatory response driven by histamine and cytokines?
Fortunately the answers to these 4 questions are: YES, YES, YES and YES! In fact, there are lots of opportunities to intervene, and slow things down. With these thoughts in mind, let’s crack on and explore some natural, drug-free nutrients.
***
YOUR 6-STEP ACTION PLAN
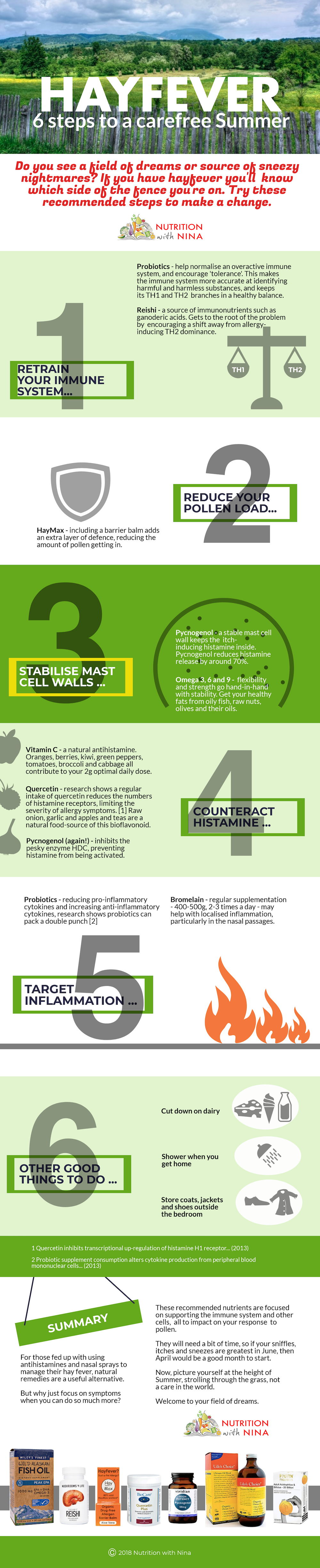
STEP 1. Retrain the immune system … Probiotics, Reishi
The immune system of a newborn baby has to learn how to be tolerant, how to distinguish between harmful and harmless substances, and how to react appropriately. The healthiest state of tolerance is achieved when the two branches of the immune system are balanced, and there is a regular, daily shift between the TH1 branch and the TH2 branch. Allergies arise when the TH2 branch dominates for most of the day.
PROBIOTICS: Exposure to probiotics, ‘good bacteria’, is a key step in the development of a tolerant immune system. Luckily, the same mechanisms exist in adults, which is why probiotics are suggested for hayfever. They help retrain the immune system. (They also increase the levels of secretory IgA. This important antibody lines the nasal passage, throat and GI tract, and helps minimise the negative effect of allergens.)
REISHI: The medicinal mushroom reishi also has a huge impact on the immune system. It’s a source of ganoderic acids and other immunonutrients, activating non-specific responses and ultimately encouraging a shift away from TH2 dominance, back to TH1-TH2 balance. [1]
STEP 2. Reduce the amount of pollen getting in … HayMax
This is one of my favourites, and it’s not even a supplement. Actually, it’s an organic barrier balm which reduces the amount of pollen getting in by more than a third. You simply rub a small amount round the rim of the nostrils, and reapply every time you blow your nose. It’s my number 1 recommendation for pregnant women and children.
STEP 3. Stabilise the mast cell walls … Omega 3, Omegas 6 and 9, Pycnogenol
OMEGA OILS: Flexibility and strength are where the power lies. As with most cells, the walls of the mast cells are made up of phospholipids. This means you need to start eating some healthy oil, particularly the omega 3 fats found in oily fish. Some good quality omega 6 and omega 9 fats wouldn’t go amiss either. They are all needed to make a healthy cell membrane. Remember, the goal is for the walls to be flexible, not too rigid and not too floppy, and a combination of cold-processed omega 3, 6, and 9 oils will help you achieve this.
PYCNOGENOL: Pycnogenol, an extract from the bark of the French maritime pine tree, is incredibly effective, stabilising cells to reduce histamine release by up to 70%.
STEP 4: Counteract histamine … Vitamin C, Quercetin, Pycnogenol
This is what most people focus on when they take anti-histamine medication. However, there are several nutrients which have a similar action in the body.
VITAMIN C: Fruits and vegetables which are naturally vitamin C-rich foods include oranges, mangoes, blueberries, raspberries, strawberries, melon, kiwi, green peppers, tomatoes, broccoli, cabbage, and fortified juices. Eat these raw where possible. 2g a day is recommended in studies, so you may want to supplement too.
QUERCETIN: Raw garlic and onions, apples and tea are good sources of quercetin. In an animal study, researchers found pre-treatment with quercetin for three weeks effectively reduced expression of the H1 histamine receptor. Normally, expression of this receptor correlates with the severity of allergy symptoms. More receptors equals more symptoms. This research suggests quercetin helps reduce the number of receptors. [2]
PYCNOGENOL: Pycnogenol also plays a role here, as it inhibits HDC, the enzyme which activates histamine. 50 – 100mg a day is a reasonable starting point.
STEP 5: Target localised inflammation … Probiotics, Bromelain
PROBIOTICS: Do you remember the cytokines? The chemical mediators released from the mast cells? They actually come in 2 flavours – pro-inflammatory and anti-inflammatory, which means you have many opportunities to impact on localised inflammation. You might enhance production of the anti-inflammatory cytokines (IL-10 and TBF-β). You might reduce production of the pro-inflammatory cytokines (IL-6 and IL-1β). Or you might do both. In their study of healthy people, researchers found the Lab4 probiotic did exactly this. [3]
BROMELAIN: You can eat pineapple, especially the core, for bromelain, although supplementing around 400-500mg, 2 to 3 times a day, could be more effective. Bromelain reduces sensitisation and inflammatory responses, particularly in nasal passages. [4]
STEP 6: Other good things to do … Cut out dairy, Shower every day, Store coats and jackets outside the bedroom.
Minimising dairy intake helps shift immune system from TH2 dominance to TH1-TH2 balance. A shower and change in storage brings less pollen into your home and bedroom.
Makes perfect sense eh?
REFERENCES
[1] https://www.mycologyresearch.com/articles/view/28 [2] https://www.ncbi.nlm.nih.gov/pubmed/23333628 [3] https://www.provenprobiotics.co.uk/proven-research/immune-system/lab4-immune-response-study [4] http://www.altmedrev.com/archive/publications/5/5/448.pdf
[…] you’ll remember pycnogenol for its potent anti-histamine actions, an essential for tackling Hayfever. Pycnogenol can stimulate the immune system, which means it is not a good supplement to take if you […]